Why Do We Have Allergies?
When scientists set out to understand a challenging and complicated problem they frequently construct models to help the process of discovery. Models help us to visualize the big picture, and to see how individual pieces of information fit together. This is true when we try to understand allergy.
Our immune system is a particularly complex bit of machinery. Its job is to monitor our internal and external environment, and when it detects a problem, eliminate the danger. It vigilantly looks out for an attack from pathogenic microbes such as bacteria and viruses, injury from various toxic substances, and cancer cells trying to get a foot hold.
When the immune system finds a problem it deals with it through a process called inflammation. Inflammation is what we experience when our immune system is doing its job; or at least believes that it is doing its job.
When we get a fever, snotty nose, and cough with a cold, these symptoms are not caused by the virus but by our immune system fighting the virus. Good thing too, because without that snotty nose the only thing we may feel is the virus eating our brain.

BaileyBio.com
When we get a thorn in our foot, the irritation, itching, redness and swelling in the area is a result of inflammation. Inflammation increases the blood supply to the area and makes the blood vessels leaky so that antibodies, blood clotting chemicals, and white blood cells can rapidly move in. The pain and itching we feel is to alert us to the thorn so that we will stop walking on it and try to get it out.
We would not last long without our immune system doing its job through inflammation, but sometimes our immune system does things that appear to have no point and seem to cause more harm than good.
The reality is, a significant percentage of the chronic medical conditions we suffer from fall under the category of chronic inflammation of unknown cause or, put another way, unknown purpose. What is our immune system thinking?
A variety of devastating autoimmune diseases such as rheumatoid arthritis and lupus certainly fit into the category of chronic inflammation with unknown purpose, but so does some neuro psychiatric and neuro degenerative diseases (such as muscular sclerosis) and of course, allergy.
What But Not Why
In medicine we are pretty good at answering the “what” questions, such as: “What chemical in the skin causes the itching and swelling when you break our in hives?” Or, “What white blood cells cause an asthma attack?” In fact, I have many big textbooks with pages of explanations and diagrams showing how our immune system reacts with harmless things like breakfast or the family dog to cause allergy misery. 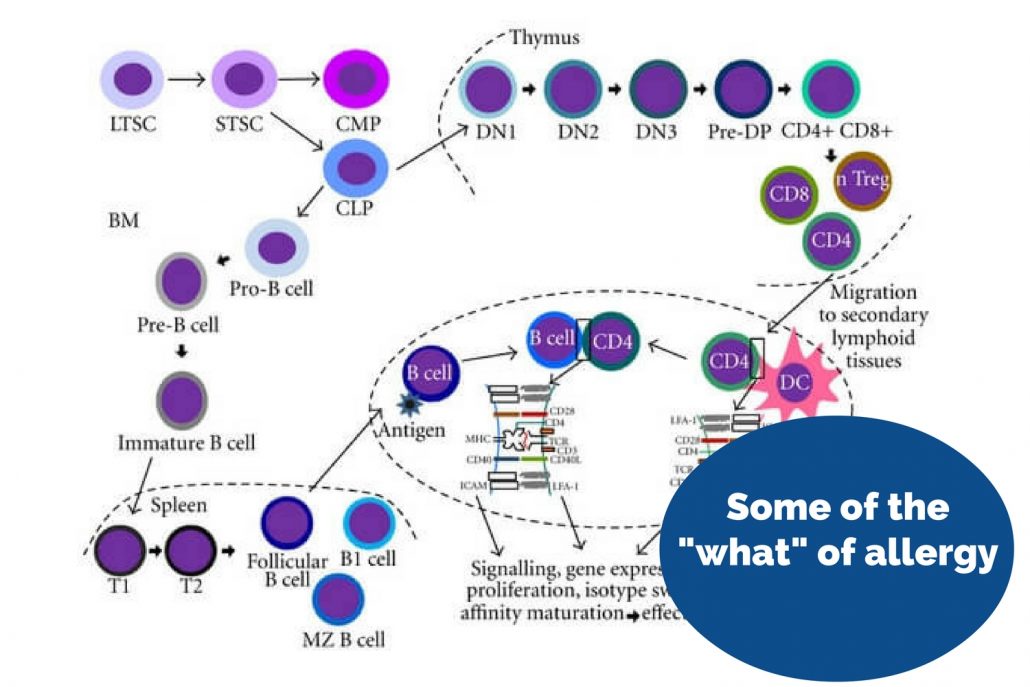
But to many, myself included, the more pressing question is “why?”. Why hives? Why asthma? Why lupus? Our sophisticated, highly developed immune system reacts, at times violently, to things that we eat, breathe or touch. Things that are, to the best of our knowledge, harmless.
A simple answer to these “why?”questions about the elusive and baffling world of chronic inflammatory disease would be to say that it is a mistake.
A very big mistake.
Millions of dollars spent on medications and doctor visits, time lost from school, work, and play, and even lives lost because of an error?
What Went Wrong and Who is To Blame?
We don’t have clear answers but we do have a large body of emerging data from research that presents some intriguing clues. In the next post (here) I will discuss a few of the current theories and models that are being proposed that will hopefully help us to unlock the mystery of “why?”.
Brian Millhollon, MD



